General Dermatology
Psoriasis
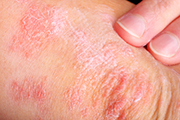 Psoriasis is a noncontagious skin disorder that most commonly appears as inflamed swollen skin lesions covered with silvery white scales. This most common type of psoriasis is called plaque psoriasis. Psoriasis comes in many different variations and degrees of severity. Different types of psoriasis display characteristics such as pus-like blisters (pustular psoriasis), severe sloughing of the skin (erythrodermic psoriasis), drop-like dots (guttate psoriasis) and smooth inflamed lesions (inverse psoriasis). The degrees of severity of psoriasis are divided into three important categories: mild, moderate and severe.
Psoriasis is a noncontagious skin disorder that most commonly appears as inflamed swollen skin lesions covered with silvery white scales. This most common type of psoriasis is called plaque psoriasis. Psoriasis comes in many different variations and degrees of severity. Different types of psoriasis display characteristics such as pus-like blisters (pustular psoriasis), severe sloughing of the skin (erythrodermic psoriasis), drop-like dots (guttate psoriasis) and smooth inflamed lesions (inverse psoriasis). The degrees of severity of psoriasis are divided into three important categories: mild, moderate and severe.
What causes Psoriasis?
No one knows what causes psoriasis, though it is generally accepted that it has a genetic component, recent studies have focused on cells called T-lymphocytes. The immune function of these cells are altered in psoriasis. Scientists believe that a person is born genetically predisposed to psoriasis. One in three people report a family history of psoriasis, but there is no pattern of inheritance. There are many cases in which children with no apparent family history of the disease will develop psoriasis.
Whether a person actually develops psoriasis may depend on something triggering its appearance. Examples of trigger factors include systemic infections such as strep throat, injury to the skin (the Koebner phenomenon), vaccinations, certain medications, and intramuscular injections or oral steroid medications.
Once something triggers a person's genetic tendency to develop psoriasis, it is thought that products of certain t-cells trigger the excessive skin cell reproduction.
What is the cycle of Psoriasis?
Skin cells are programmed to follow two possible programs: normal growth or wound healing. In a normal growth pattern, skin cells are created in the basal cell layer, and then move up through the epidermis to the stratum corneum, the outermost layer of the skin. Dead cells are shed from the skin at about the same rate as new new cells are produced, maintaining a balance. This normal process takes about 28 days from cell birth to death.
When skin is wounded, a wound healing program is triggered, also known as regenerative maturation. Cells are produced at a much faster rate, theoretically to replace and repair the wound. There is also an increased blood supply and localized inflammation. In many ways, psoriatic skin is similar to skin healing from a wound or reacting to a stimulus such as infection.
Lesional psoriasis is characterized by cell growth in the alternate growth program. Although there is no wound at a psoriatic lesion, skin cells (called keratinocytes) behave as if there is. These keratinocytes switch from the normal growth program to regenerative maturation. Cells are created and pushed to the surface in as little as 2-4 days, and the skin cannot shed the cells fast enough. The excessive skin cells build up and form elevated, scaly lesions. The white scale (called plaque) that usually covers the lesion is composed of dead skin cells, and the redness of the lesion is caused by increased blood supply to the area of rapidly dividing skin cells.
How does one live with Psoriasis?
Psoriasis can be very painful, but the pain is more than skin deep. The emotions suffer as well. It presents people with physical limitations, disfiguration, and its tedious, daily care always demands too much time. Embarrassment, frustration, fear, and depression are common. In extreme cases, a loss of self-esteem results in a complete withdrawal from society.
What treatments are available for Psoriasis?
Various kinds of temporary relief are available, and they work with varying degrees of success. A variety of topically applied medications can help control limited psoriasis. Localized psoriasis can also be managed with a series of brief laser treatments. For more severe psoriasis, oral medications or the newer injectable “biologic agents” can be prescribed. Sunlight exposure can also be effective. You can discuss treatment options during your office visit.
![]() To learn more about our General Dermatology services or to schedule an appointment, please contact our office.
To learn more about our General Dermatology services or to schedule an appointment, please contact our office.
